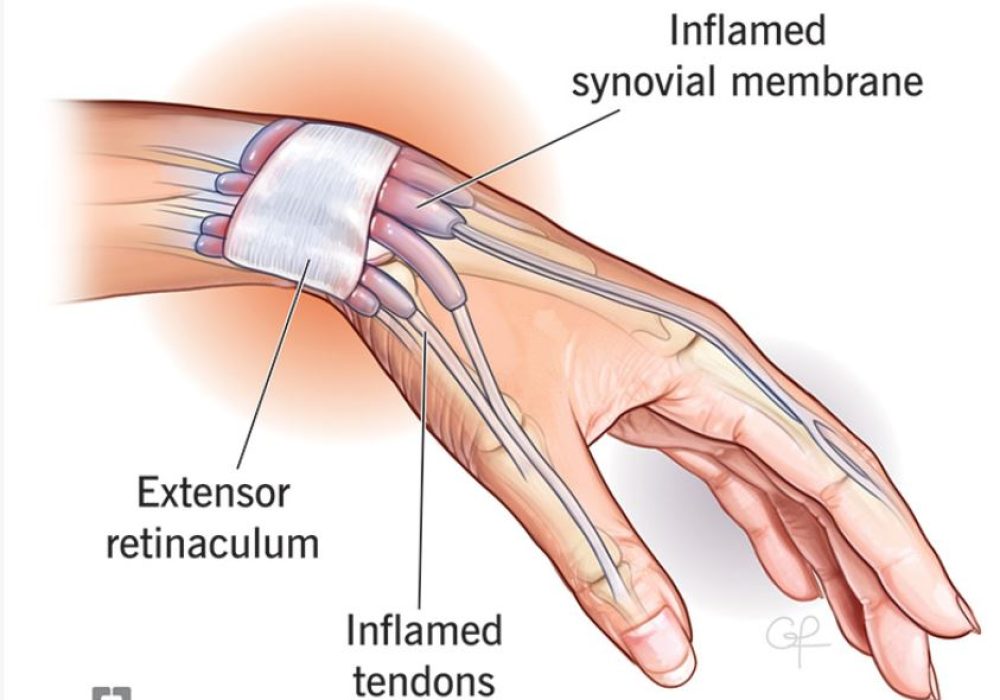
Extensor Tenosynovectomy
Extensor tenosynovectomy is a surgical procedure that involves the removal of inflamed or thickened synovial tissue surrounding the extensor tendons in the hand, wrist, or forearm. Extensor tendons are responsible for straightening the fingers, thumb, and wrist, playing a vital role in functional hand movements such as releasing objects, typing, or playing musical instruments. These tendons are covered by a protective sheath lined with synovium, a thin membrane that produces fluid to reduce friction and facilitate smooth tendon gliding.
When the synovium becomes chronically inflamed or thickened—a condition called tenosynovitis—it can restrict tendon motion, cause pain, swelling, and, if untreated, potentially damage or rupture the tendon. Extensor tenosynovectomy is performed to remove this diseased tissue, restore tendon mobility, and relieve symptoms.
Tendon Surgery
Make Your Appointment
Causes of Extensor Tenosynovitis
The condition leading to extensor tenosynovectomy may develop due to several reasons:
Rheumatoid arthritis: Chronic autoimmune inflammation is one of the most common causes, leading to excessive synovial proliferation that can erode tendons.
Inflammatory conditions: Other connective tissue diseases can also affect tendon sheaths.
Repetitive strain or overuse: Frequent wrist and finger movements may irritate the extensor tendons.
Trauma: Injuries around the wrist or hand may trigger synovial thickening.
Infections: Though less common, infections can damage tendon sheaths and cause long-term problems.
Symptoms
Patients with extensor tenosynovitis often report:
Persistent swelling on the back of the wrist or hand.
Pain or discomfort, especially during extension of the wrist or fingers.
Stiffness and reduced ability to straighten fingers or wrist.
A feeling of tightness or resistance when moving the affected tendons.
In severe cases, snapping, tendon rupture, or visible deformity.
Indications for Surgery
Extensor tenosynovectomy is considered when:
Non-surgical treatments (rest, splinting, medications, or corticosteroid injections) fail to provide relief.
There is progressive tendon dysfunction due to rheumatoid arthritis or similar conditions.
Swelling or pain interferes significantly with daily hand function.
Imaging or clinical examination shows that tendons are at risk of rupture from chronic synovial invasion.
The Surgical Procedure
The surgery is usually performed under regional block anesthesia or general anesthesia, depending on the extent of involvement and patient needs.
Incision: A carefully placed incision is made over the affected extensor tendons, often on the back of the hand or wrist. The incision is aligned with natural skin creases to reduce visible scarring.
Exposure: The extensor tendons and their sheaths are gently exposed.
Removal of diseased synovium: The surgeon excises the thickened or inflamed synovial tissue encasing the tendons. Diseased tissue is meticulously cleared while preserving healthy tendon structures.
Inspection of tendons: The surgeon assesses each tendon for thinning, fraying, or rupture. If needed, tendon repair or grafting may be performed at the same time.
Closure: Once the tendons glide freely and swelling tissue is removed, the incision is closed with sutures, and a sterile dressing is applied.
In patients with rheumatoid arthritis, multiple tendons may be involved, so a more extensive tenosynovectomy may be carried out to preserve overall hand function.
Postoperative Care and Rehabilitation
Recovery after extensor tenosynovectomy depends heavily on careful postoperative management and therapy.
Immobilization: A protective splint or dressing is often applied initially to allow the wound to heal.
Early mobilization: Once safe, patients are encouraged to begin gentle finger and wrist movements under the supervision of a hand therapist to prevent stiffness.
Hand therapy: Structured physiotherapy exercises are essential for restoring strength, flexibility, and tendon gliding.
Scar management: Techniques such as massage or silicone therapy may reduce scar tightness.
Pain and swelling control: Ice, elevation, and prescribed medications are used to manage postoperative discomfort.
Risks and Complications
Like all surgical procedures, extensor tenosynovectomy carries some risks:
Infection of the wound.
Recurrence of synovitis, particularly in chronic inflammatory conditions.
Scar formation leading to stiffness or adhesions.
Damage to nearby tendons, nerves, or blood vessels.
Incomplete recovery of motion if the disease process is advanced.
Rarely, tendon rupture if the tendons are severely weakened.
Outcomes
The outcome of extensor tenosynovectomy is generally positive, particularly when performed early before irreversible tendon damage occurs. Patients often experience:
Relief from pain and swelling.
Improved tendon motion and function.
Prevention of tendon rupture in inflammatory conditions.
However, in patients with ongoing diseases like rheumatoid arthritis, recurrence of synovitis is possible, and long-term management of the underlying condition is equally important. The success of surgery also relies heavily on postoperative rehabilitation and the patient’s adherence to therapy.
Conclusion
Extensor tenosynovectomy is a valuable surgical procedure for managing chronic tenosynovitis of the extensor tendons when conservative treatments are not effective. By removing diseased synovium, the procedure relieves pain, restores tendon movement, and protects tendons from further damage or rupture. While risks exist, careful surgical technique, combined with dedicated rehabilitation, usually leads to improved function and quality of life. For patients with conditions like rheumatoid arthritis, extensor tenosynovectomy plays a crucial role in preserving long-term hand function.
