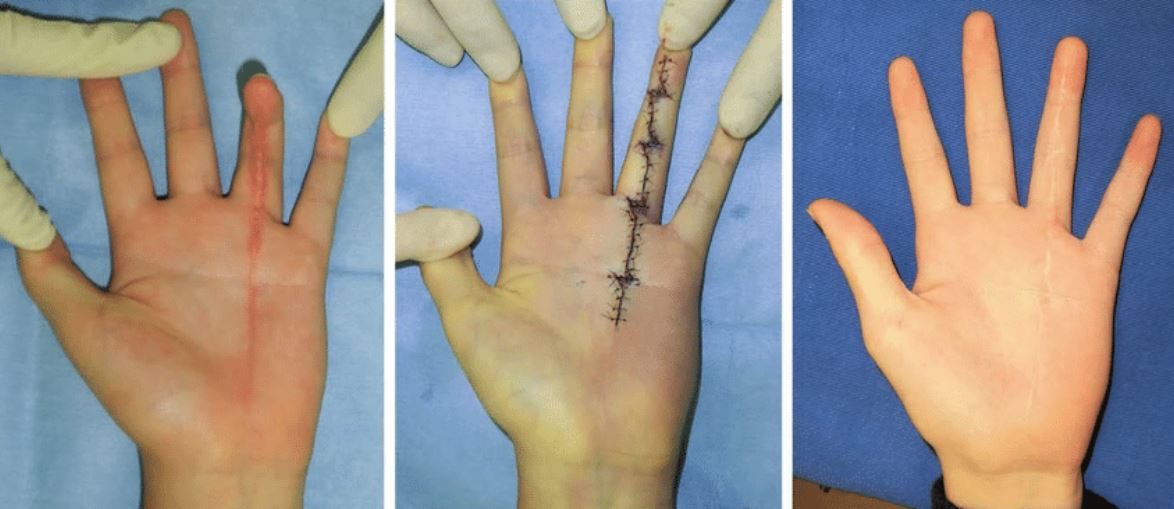
Hand Contracture
Traumatic contractures of the small joints in the hand can develop after either injury or surgery. Once the limiting scar tissue is mature (usually after 3 months from the last event) no amount of therapy will be able increase motion.
MEDICAL HISTORY
Patients typically complain of pain, stiffness, weakness, and loss of hand function. The doctor will ask questions to uncover all the events that led up to or contributed to the development of the contracture. Knowing how the contracture formed is the key in planning to eliminate the contracture.
EXAMINATION
Specific measurements will be made of both the passive (someone else moves the joint by pushing on it) and active (joint is moved by its own tendons) motion of each involved joint. Tests will be done to evaluate the function of the relevant tendons.
ADDITIONAL TESTS
Plain x-rays will show any underlying joint damage that might make achieving good motion more difficult.
TREATMENT OPTIONS
- NON-OPERATIVE
- SURGICAL RELEASE
NON-OPERATIVE
CONSISTS OF
Outpatient therapy
FEATURES
Stretching exercises and splints
ADVANTAGES
Avoids Surgery
DISADVANTAGES
Only effective early when scar tissue is immature.
SURGICAL RELEASE
CONSISTS OF
Surgically excising scar tissue from around joints and tendons.
HAND PROBLEMS
- Fractures and Dislocations in Hand
- Metacarpal & Phalangeal fractures
- Ligamentous injuries of fingers & Thumb
- Dislocations of finger joints
- Swellings of Fingers & Hand
- Compartment Syndrome
- Mucous cyst
- Ganglion cyst / Retinacular Cyst
- GCT of Tendon sheath
- Enchondroma (Benign Bone Tumor)
- Squamous cell carcinoma
- Dupuytrens Contracture
- Post Traumatic Contracture
- Post Burn Contractures of fingers
- Volkmann Ischemic Contracture
- Stiff Fingers & CRPS
- Stiff joints of fingers and hand
- Osteoarthritis of Hand
- Finger joint arthritis
- Thumb Basal joint arthritis
- Acute Infections of Hand
- Finger Pulp Infection (Felon)
- Nail Fold Infection (Paronychia)
- Finger Infection (Flexor Tenosynovitis)
- Palm Infection (Deep Spaces of Hand infection)
- Joint Infections in Hand & Wrist (Septic Arthritis)
- Human & Animal bite injuries to hand
- Diabetic Hand Infections
- Bacterial / Fungal / Atypical Hand infections in immunocompromised patients
- Subungual Hematoma
- Nail bed injury
- Nail Deformities
- Glomus tumor
Make Your Appointment
FEATURES
Outpatient surgery, patient actively participates in evaluation at time of surgery.
ADVANTAGES
Maximum correction possible, used when previous scar is mature.
DISADVANTAGES
Correction proportionate to original problem, some new scar tissue forms after surgery
RECOVERY
Patients must be very committed to their treatment to choose surgical correction of a contracture. Intense outpatient rehabilitation begins immediately after surgery. Patients must perform motion exercises every hour on the hour when awake, seven days a week. Sutures are taken out after 2 weeks in the office. Splints are used at night and sometimes during the day to preserve increases in motion. New scar tissue gradually forms and matures over about a 3-month period after surgery. When therapy is finished after the scar matures patients will have some percentage of motion that is still less than the freedom achieved on the day of surgery.
