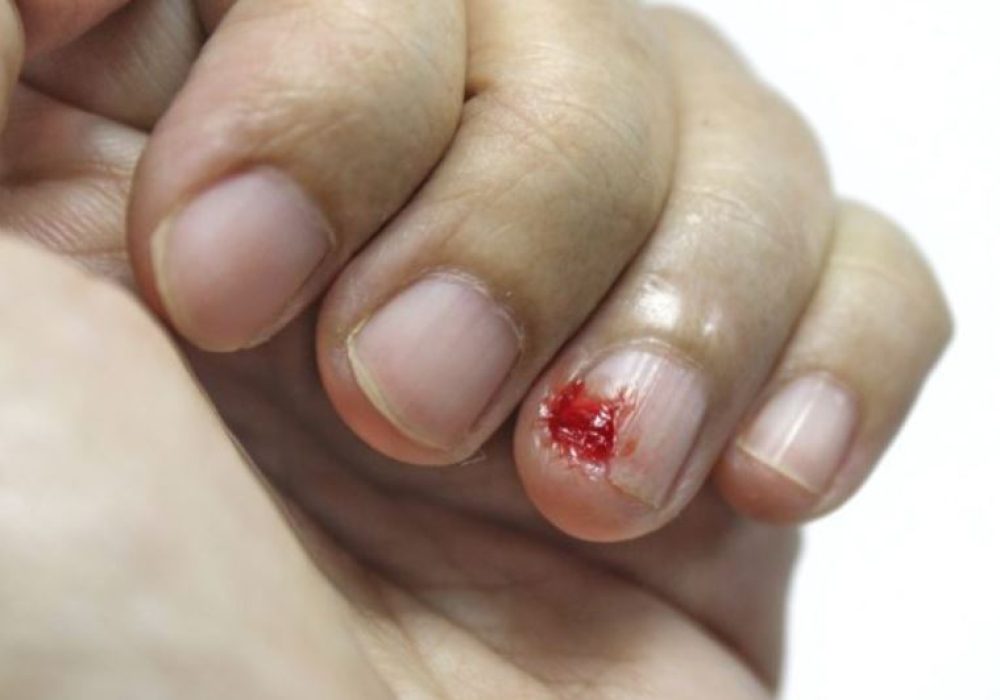
Nail bed injury
Nail bed (nailbed) injuries are common, with fingertip injuries being the most commonly seen hand injuries. [1, 2] The fingertip is frequently injured because it is the point of interaction between the body and one’s surroundings in the majority of activities performed on a daily basis, and it is the most distal portion of the upper extremities. Besides having long-term cosmetic consequences, injuries to the nail can affect daily living. [3] The nail provides protection for the fingertip, offers the ability to pick up small objects, and plays a role in tactile sensation. It serves as a counterforce when the finger pad touches an object; two-point discrimination distance widens substantially with removal of a nail.
Injuries to the nail bed are frequently caused by crushing trauma (eg, from a hammer blow). [5] About 25% of nail bed injuries involve the finger being crushed by a door (most commonly a car door). Crush injuries squeeze the soft tissue of the nail bed between the nail and the distal phalanx. This may result in a simple subungual hematoma or a simple or stellate laceration. Saws, knives, drills, moving belts, and lawnmowers are also common causes of nail bed injuries. Crush and avulsion injuries (see the image below), as well as injuries associated with distal phalanx fractures, have a worse prognosis.
Blunt trauma to the fingertip and nail bed must be appropriately treated to prevent secondary deformities and reduce the need for subsequent reconstruction. [6] Delayed or inadequate treatment can result in negative functional and cosmetic outcomes. The peak incidence of fingertip and nail bed injuries is between the ages of 4 and 30 years. According to Chang et al, 10% of such accidents are treated in the emergency department. In the case of fingertip injuries, the nail bed is injured in 15-24% of cases. [7]
The injured finger can usually be examined without anesthesia, though children or those in severe pain may require a digital block first. A complete examination of sensation (performed prior to a digital block), motor function, and vascular supply is necessary. It is important to observe the posture of the fingers; to look for any presence of deformities signifying fracture, dislocation, or tendon avulsion; and to be alert to the presence of glass, wood, metal, or other foreign-body fragments.
Depending on the extent of injury, radiologic evaluation with anteroposterior, lateral, and oblique views of the injured finger(s) may be useful to rule out foreign bodies and fractures or dislocations of the distal finger. [4]
Prophylactic administration of antibiotics is indicated, depending on the mechanism and extent of injury (eg, crush injuries as distinct from human bites or animal bites. Many clinicians prescribe a first-generation cephalosporin when bone or joint is exposed below a nail bed injury.
For small (< 25% of the nail bed) and painless subungual hematomas, no intervention is required, because the hematoma will eventually reabsorb. If the subungual hematoma covers more than 25% of the nailbed or is causing pain, the patient should be offered evacuation via trephination or nail removal.
HAND PROBLEMS
- Fractures and Dislocations in Hand
- Metacarpal & Phalangeal fractures
- Ligamentous injuries of fingers & Thumb
- Dislocations of finger joints
- Swellings of Fingers & Hand
- Compartment Syndrome
- Mucous cyst
- Ganglion cyst / Retinacular Cyst
- GCT of Tendon sheath
- Enchondroma (Benign Bone Tumor)
- Squamous cell carcinoma
- Dupuytrens Contracture
- Post Traumatic Contracture
- Post Burn Contractures of fingers
- Volkmann Ischemic Contracture
- Stiff Fingers & CRPS
- Stiff joints of fingers and hand
- Osteoarthritis of Hand
- Finger joint arthritis
- Thumb Basal joint arthritis
- Acute Infections of Hand
- Finger Pulp Infection (Felon)
- Nail Fold Infection (Paronychia)
- Finger Infection (Flexor Tenosynovitis)
- Palm Infection (Deep Spaces of Hand infection)
- Joint Infections in Hand & Wrist (Septic Arthritis)
- Human & Animal bite injuries to hand
- Diabetic Hand Infections
- Bacterial / Fungal / Atypical Hand infections in immunocompromised patients
- Subungual Hematoma
- Nail bed injury
- Nail Deformities
- Glomus tumor
Make Your Appointment
Lacerations to the nail bed should be repaired with 6-0 or smaller absorbable sutures. Minimal to no debridement should be performed, because aggressive debridement may cause undue tension on the repair and may result in scarring.
A digital block of 1% lidocaine hydrochloride without epinephrine provides anesthesia of sufficient duration for most repairs. For longer repairs, bupivacaine extends anesthesia time 4-8 hours. Children may require procedural sedation and analgesia.
During repair of avulsed nails and nail beds, if the nail is detached proximally, it must be removed to inspect for any damage to the nail bed.
