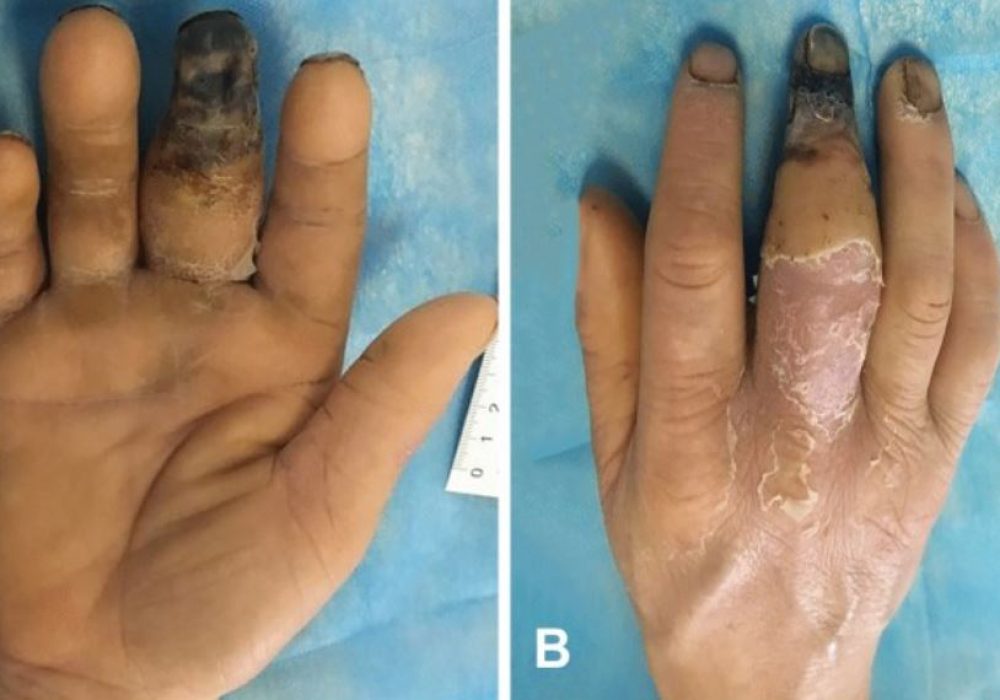
Diabetic Hand Infections
Diabetic hand infections are serious complications that occur more frequently and with greater severity in individuals with diabetes. These infections often involve soft tissues and can lead to significant morbidity, disability, and sometimes require surgical intervention. Poor glycemic control, delayed treatment, and compromised immune response contribute to the increased risk and severity of these infections. Common presentations include swelling, pain, redness, and sometimes abscess formation or necrosis. Prompt medical attention, proper wound care, and strict blood sugar management are essential to prevent progression and improve outcomes. In some regions, a severe form known as Tropical Diabetic Hand Syndrome is recognized, characterized by rapid infection spread and tissue destruction. Early diagnosis and multidisciplinary care are key to reducing complications and preserving hand function.
Diabetic Hand Infections: Overview
- Diabetic hand infections are a significant cause of morbidity and disability among diabetic patients.
- These infections range from cellulitis and abscesses to severe necrotizing fasciitis.
- They often require surgical intervention, including debridement and sometimes amputation.
- The risk of infection and severity is increased due to impaired immunity, poor blood sugar control, and vascular complications associated with diabetes.
Risk Factors and Presentation
- Delay in seeking medical care after symptom onset significantly increases the risk of amputation and the need for multiple surgeries.
- Infections caused by Gram-negative bacteria are associated with more complicated clinical courses requiring multiple procedures.
- Many patients present late, often after self-treatment or inadequate initial care.
- Common symptoms include swelling, pain, redness, and sometimes formation of blebs or necrotic tissue.
- Some patients may have no clear history of trauma, with spontaneous infections occurring due to unnoticed minor injuries.
Microbiology
- Both Gram-positive and Gram-negative organisms are implicated.
- Staphylococcal species, including coagulase-negative Staphylococci and Staphylococcus aureus, are common Gram-positive pathogens.
- Klebsiella and Escherichia coli are frequent Gram-negative isolates.
- Gram-negative infections tend to require more aggressive and repeated surgical management.
Management
- Early and aggressive surgical debridement is critical.
- Empirical antibiotic therapy is started on admission and adjusted based on culture and sensitivity results.
- Multiple surgical procedures may be necessary, including incision and drainage, debridement, skin grafts, and flap coverage.
- Physiotherapy should begin within 48 to 72 hours post-surgery to preserve hand function.
- Strict glycemic control and management of comorbidities are important adjuncts to treatment.
HAND PROBLEMS
- Fractures and Dislocations in Hand
- Metacarpal & Phalangeal fractures
- Ligamentous injuries of fingers & Thumb
- Dislocations of finger joints
- Swellings of Fingers & Hand
- Compartment Syndrome
- Mucous cyst
- Ganglion cyst / Retinacular Cyst
- GCT of Tendon sheath
- Enchondroma (Benign Bone Tumor)
- Squamous cell carcinoma
- Dupuytrens Contracture
- Post Traumatic Contracture
- Post Burn Contractures of fingers
- Volkmann Ischemic Contracture
- Stiff Fingers & CRPS
- Stiff joints of fingers and hand
- Osteoarthritis of Hand
- Finger joint arthritis
- Thumb Basal joint arthritis
- Acute Infections of Hand
- Finger Pulp Infection (Felon)
- Nail Fold Infection (Paronychia)
- Finger Infection (Flexor Tenosynovitis)
- Palm Infection (Deep Spaces of Hand infection)
- Joint Infections in Hand & Wrist (Septic Arthritis)
- Human & Animal bite injuries to hand
- Diabetic Hand Infections
- Bacterial / Fungal / Atypical Hand infections in immunocompromised patients
- Subungual Hematoma
- Nail bed injury
- Nail Deformities
- Glomus tumor
Make Your Appointment
Outcomes and Prognosis
- Delay in presentation (even by a few days) significantly increases the risk of amputation and multiple surgeries.
- Patients with Gram-negative infections are more likely to require multiple procedures.
- Presence of comorbidities, duration of diabetes, HbA1c, and random blood sugar levels at admission do not show a consistent association with outcomes.
- Mortality can occur in severe cases, especially with necrotizing infections and systemic complications like sepsis and acute kidney injury.
Prevention and Awareness
- Early recognition of hand infections in diabetic patients is essential.
- Patients and healthcare providers should be educated about the importance of prompt medical evaluation for hand symptoms.
- Avoidance of self-treatment and traditional remedies that delay proper care is critical.
- Regular monitoring and control of blood glucose levels may reduce the risk of infections.
Diabetic hand infections require prompt diagnosis and aggressive management to prevent serious complications such as amputation and prolonged hospitalization. Awareness of risk factors, early presentation, and appropriate surgical and medical treatment are key to improving patient outcomes and preserving hand function.
Diabetic hand infections represent a challenging clinical problem due to the unique pathophysiological changes in diabetic patients. Diabetes mellitus impairs the immune system, reduces blood flow, and delays wound healing, making the hands particularly vulnerable to infections. Even minor injuries can rapidly progress to severe infections if not treated promptly.
Pathophysiology
In diabetes, chronic hyperglycemia leads to:
- Microvascular and macrovascular disease: Reduced blood supply impairs delivery of immune cells and antibiotics to the infected site.
- Neuropathy: Loss of sensation increases the risk of unnoticed injuries.
- Impaired immune response: Dysfunctional neutrophil activity and reduced chemotaxis hinder infection control.
- Delayed wound healing: High blood sugar levels interfere with collagen synthesis and tissue repair.
Common Types of Diabetic Hand Infections
- Cellulitis: Diffuse inflammation of the skin and subcutaneous tissues.
- Abscess: Localized collection of pus requiring drainage.
- Tenosynovitis: Infection of the tendon sheaths causing pain and restricted movement.
- Necrotizing fasciitis: A life-threatening infection causing rapid tissue necrosis.
- Tropical Diabetic Hand Syndrome (TDHS): A severe form seen mainly in tropical regions, characterized by swelling, ulceration, and gangrene.
Clinical Features
Patients with diabetic hand infections may present with:
- Pain, swelling, and redness of the hand or fingers.
- Warmth and tenderness over the affected area.
- Limited range of motion due to pain or swelling.
- Presence of pus, blisters, or necrotic tissue.
- Systemic symptoms such as fever, chills, and malaise in advanced cases.
Treatment Strategies
Medical Management
- Antibiotics: Empirical broad-spectrum antibiotics covering both Gram-positive and Gram-negative bacteria are initiated promptly. Therapy is tailored based on culture results.
- Glycemic control: Optimizing blood sugar levels is crucial to enhance immune function and wound healing.
- Supportive care: Pain management, hydration, and nutritional support.
Surgical Management
- Early and aggressive surgical intervention is often necessary.
- Procedures include incision and drainage of abscesses, debridement of necrotic tissue, and in severe cases, amputation.
- Reconstructive surgeries such as skin grafts or flap coverage may be required to restore hand function.
- Postoperative physiotherapy is essential to prevent stiffness and maintain mobility.
Patient Education and Prevention
- Maintain good hand hygiene and skin care.
- Inspect hands regularly for cuts, blisters, or signs of infection.
- Avoid self-medication and seek prompt medical attention for any hand injury or infection.
- Control blood sugar levels through diet, medication, and regular monitoring.
- Regular follow-up with healthcare providers to manage diabetes and prevent complications.
Conclusion
Diabetic hand infections are a serious and potentially debilitating complication of diabetes that require prompt recognition and aggressive management. Due to impaired immunity, poor blood circulation, and delayed wound healing associated with diabetes, these infections can progress rapidly, leading to severe tissue damage, functional impairment, and even amputation if not treated early. Effective management involves a combination of timely surgical intervention, appropriate antibiotic therapy, strict glycemic control, and comprehensive rehabilitation. Patient education and awareness are equally important to encourage early presentation and prevent infection. With multidisciplinary care and vigilant monitoring, the risks of complications can be minimized, preserving hand function and improving quality of life for diabetic patients.
