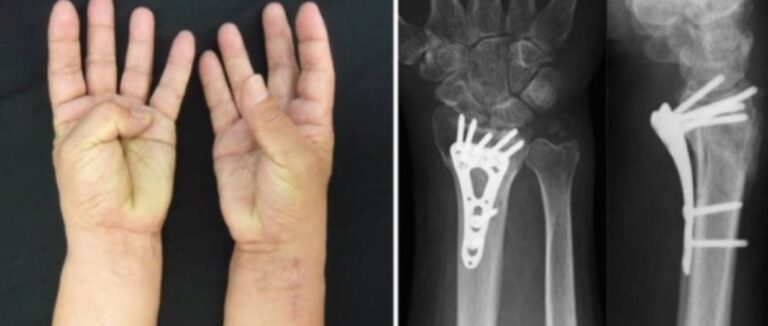
Flexor Pollicis longus
Flexor pollicis longus (FPL) tendon rupture is a significant injury that affects the function of the thumb, leading to impaired hand dexterity and strength. The FPL tendon is responsible for flexing the distal phalanx of the thumb, enabling essential movements such as pinching and gripping. When this tendon ruptures, patients experience difficulty or inability to flex the thumb, which can severely impact daily activities and hand function.
Anatomy and Function of the Flexor Pollicis Longus Tendon
The FPL tendon originates from the anterior surface of the radius and the interosseous membrane in the forearm. It travels through the carpal tunnel and inserts into the base of the distal phalanx of the thumb. This anatomical positioning allows the FPL to flex the thumb’s interphalangeal joint, a critical movement for fine motor skills. The tendon is surrounded by a synovial sheath that facilitates smooth gliding during thumb movements.
Causes and Mechanisms of FPL Rupture
FPL tendon rupture can occur due to various causes, including trauma, attrition, and iatrogenic injury. Traumatic ruptures often result from penetrating injuries or fractures involving the distal radius or scaphoid bones. For example, a scaphoid fracture can lead to attritional wear of the FPL tendon over bony prominences or osteophytes, eventually causing rupture. This is sometimes referred to as a Mannerfelt lesion, particularly in patients with rheumatoid arthritis (RA), where chronic inflammation and joint deformities predispose the tendon to rupture.
Tendon Problems
- Jersey Finger
- Zone II Flexor tendon injury
- Spaghetti Wrist
- Mallet Finger
- Swan neck Deformity
- Boutonniere Deformity
- Boxers Knuckle
- ECU Subluxation
- fight-bite-injury
- Extensor Tenosynovitis
- Flexor Tenosynovitis
- FCR Tendinitis
- FCU Tendinitis
- ECU tendinitis
- Calcific Tendinitis
- EPL Rupture
- Mannerfelt Syndrome
- Vaughan Jackson Syndrome
- Tendon Adhesions
Make Your Appointment
Iatrogenic causes are also notable, especially following surgical interventions such as volar plating for distal radius fractures. The hardware used in these procedures can irritate or directly damage the FPL tendon, leading to delayed rupture. This complication, although rare, is well-documented and requires careful surgical technique and postoperative monitoring.
Spontaneous ruptures, though less common, may occur in the context of systemic diseases like RA or due to degenerative changes in the tendon itself. Inflammatory processes weaken the tendon structure, making it more susceptible to rupture even without significant trauma.
Clinical Presentation and Diagnosis
Patients with FPL rupture typically present with an inability to flex the distal phalanx of the thumb. They may report a sudden loss of thumb function, often accompanied by pain or a snapping sensation at the time of injury. On physical examination, the absence of active flexion at the interphalangeal joint of the thumb is a key finding. The thumb may appear extended and stiff, and patients often struggle with tasks requiring pinch grip.
Diagnosis is primarily clinical but is supported by imaging studies. Ultrasound can visualize tendon discontinuity and assess the extent of injury. Magnetic resonance imaging (MRI) provides detailed images of soft tissue structures and is useful in chronic or complex cases. Radiographs are essential to identify associated fractures or bony abnormalities that may contribute to tendon rupture.
Treatment Options
Prompt surgical repair is the standard of care for FPL tendon rupture to restore thumb function and prevent long-term disability. The timing of surgery is crucial; early intervention generally leads to better outcomes. Surgical options depend on the nature and chronicity of the rupture.
Primary Repair: In acute cases where the tendon ends are viable and can be approximated without tension, direct end-to-end repair is preferred. This approach aims to restore the tendon’s continuity and function with minimal delay.
Tendon Grafting or Transfer: In chronic ruptures or cases where the tendon ends are retracted or degenerated, primary repair may not be feasible. Tendon grafts, often harvested from the palmaris longus or other donor tendons, can bridge the gap. Alternatively, tendon transfers, such as using the flexor digitorum superficialis of the ring finger, may be performed to restore thumb flexion.
Management of Associated Conditions: When FPL rupture occurs secondary to fractures or hardware irritation, addressing the underlying cause is essential. This may involve hardware removal, fracture fixation, or debridement of osteophytes to prevent recurrence.
Postoperative Care and Rehabilitation
Rehabilitation following FPL repair is critical to optimize functional recovery. Early controlled mobilization protocols are often employed to prevent tendon adhesions and stiffness while protecting the repair site. However, excessive movement too soon can increase the risk of rerupture.
Edema control, splinting, and gradual range-of-motion exercises are integral components of postoperative care. Physical therapy focuses on restoring strength, flexibility, and coordination of the thumb and hand. The rehabilitation timeline varies depending on the repair type and patient factors but generally spans several weeks to months.
Complications and Prognosis
Complications following FPL tendon rupture and repair include rerupture, adhesion formation, stiffness, and reduced range of motion. Careful surgical technique and adherence to rehabilitation protocols minimize these risks. In cases related to systemic diseases like RA, ongoing management of the underlying condition is necessary to prevent further tendon damage.
The prognosis for FPL tendon rupture is generally favorable with timely and appropriate treatment. Most patients regain significant thumb function, enabling them to perform daily activities and occupational tasks. Delayed diagnosis or treatment can lead to permanent functional impairment and may require more complex reconstructive procedures.
Special Considerations in Rheumatoid Arthritis
Rheumatoid arthritis patients are particularly susceptible to FPL tendon rupture due to chronic synovitis and joint deformities. The Mannerfelt lesion describes attritional rupture of the FPL tendon over a bony spur on the scaphoid, a common complication in RA. Management in these patients involves not only tendon repair but also addressing joint inflammation and deformities to prevent recurrence.
Conclusion
Flexor pollicis longus tendon rupture is a debilitating injury that significantly impairs thumb function. Understanding the anatomy, causes, clinical presentation, and treatment options is essential for effective management. Early diagnosis and surgical repair, combined with appropriate rehabilitation, offer the best chance for restoring hand function and improving patient quality of life. Awareness of risk factors such as trauma, fractures, surgical complications, and systemic diseases like rheumatoid arthritis is crucial in preventing and managing this condition.
Flexor Pollicis Longus (FPL) Tendon Rupture: An In-Depth
Overview
Flexor pollicis longus (FPL) tendon rupture is a serious injury that compromises the ability to flex the thumb, which is essential for hand dexterity and grip strength. This condition can arise from trauma, surgical complications, or degenerative diseases, and often requires surgical intervention to restore function.
Anatomy and Function of the FPL Tendon
- The FPL tendon originates from the anterior surface of the radius and the interosseous membrane.
- It passes through the carpal tunnel and inserts on the base of the distal phalanx of the thumb.
- Its primary function is to flex the interphalangeal joint of the thumb, enabling fine motor tasks such as pinching and grasping.
- The tendon is enclosed in a synovial sheath that facilitates smooth gliding during thumb movements.
Causes and Mechanisms of FPL Rupture
- Trauma: Direct injury or fractures of the distal radius or scaphoid can cause rupture.
- Attritional Rupture: Chronic irritation or rubbing of the tendon over bony prominences or hardware (e.g., volar plates) can lead to gradual wear and rupture.
- Iatrogenic Injury: Surgical procedures, especially volar plate fixation for distal radius fractures, may inadvertently damage or irritate the FPL tendon.
- Systemic Diseases: Conditions like rheumatoid arthritis (RA) cause chronic inflammation and joint deformities, increasing the risk of spontaneous tendon rupture (Mannerfelt lesion).
- Degenerative Changes: Age-related tendon degeneration can predispose to rupture even without trauma.
Clinical Presentation and Diagnosis
- Patients typically present with:
- Sudden loss of thumb flexion.
- Inability to flex the distal phalanx of the thumb.
- Pain or a snapping sensation at the time of injury.
- Physical examination reveals:
- Absence of active flexion at the thumb’s interphalangeal joint.
- Thumb held in extension or neutral position.
- Diagnostic tools include:
- Ultrasound: Visualizes tendon discontinuity and assesses injury extent.
- MRI: Provides detailed soft tissue imaging, useful in chronic or complex cases.
- X-rays: Identify associated fractures or hardware positioning that may contribute to rupture.
Treatment Approaches
- Surgical Repair: The mainstay of treatment to restore thumb function.
- Primary Repair: Suitable for acute ruptures with viable tendon ends; involves direct end-to-end suturing.
- Tendon Grafting: Used in chronic ruptures or when tendon ends are retracted; commonly uses the palmaris longus tendon as a graft.
- Tendon Transfer: Alternative grafts include flexor digitorum superficialis or extensor indicis proprius tendons.
- Hardware Management: Removal of volar plates or other implants that may cause tendon irritation.
- Addressing Underlying Causes: Treatment of fractures, osteophytes, or systemic diseases to prevent recurrence.
Postoperative Care and Rehabilitation
- Immobilization of the wrist and thumb in a protective splint or cast initially.
- Gradual introduction of controlled passive and active range-of-motion exercises to prevent adhesions.
- Pain management and infection prevention are critical in the early postoperative period.
- Physical therapy focuses on restoring strength, flexibility, and coordination.
- Rehabilitation duration varies but typically spans several months for optimal recovery.
Complications and Prognosis
- Potential complications include:
- Tendon rerupture.
- Adhesion formation leading to stiffness.
- Reduced range of motion.
- Infection or wound healing issues.
- Prognosis is generally good with timely surgical intervention and adherence to rehabilitation protocols.
- Delayed treatment may result in permanent functional impairment requiring complex reconstructive surgery.
Special Considerations: FPL Rupture After Volar Plate Fixation
- Volar plate fixation for distal radius fractures is a common cause of FPL tendon rupture due to the proximity of the tendon to the hardware.
- The incidence of rupture after volar plating ranges from 0.7% to 10%.
- Surgical management involves:
- Removal of the volar plate.
- Tenolysis to free the tendon from adhesions.
- Reconstruction using a palmaris longus tendon graft.
- Early plate removal (within 6–12 months) may reduce rupture risk, but evidence is mixed.
- Postoperative rehabilitation is crucial to regain wrist and thumb function.
Case Series Insights
- Patients with FPL rupture following volar plate fixation showed significant functional improvement after surgical reconstruction with palmaris longus tendon grafts.
- No major postoperative complications such as infection or wound dehiscence were reported.
- Rehabilitation and follow-up demonstrated gradual restoration of thumb flexion and wrist range of motion.
- Multidisciplinary care involving orthopedic surgeons, plastic surgeons, and rehabilitation specialists optimizes outcomes.
Conclusion
Flexor pollicis longus tendon rupture is a debilitating injury that significantly impairs hand function. It can result from trauma, surgical complications, or systemic diseases. Early diagnosis and surgical repair, often involving tendon grafting, are essential to restore thumb flexion and hand dexterity. Postoperative rehabilitation plays a vital role in recovery, and careful management of underlying causes helps prevent recurrence. Awareness of this condition, especially in patients with distal radius fractures treated with volar plates, is critical for timely intervention and improved patient outcomes.
