Distal Humeral Fracture
Distal Humeral Fractures are traumatic injuries involving the epicondyles, the trochlea, the capitellum, and the metaphysis of the distal humerus. They are often the result of high-energy trauma, such as road traffic accidents or a fall from a height. In the elderly, they may occur as a domestic accident .
Risk Factors
Attributes, characteristics or activities that increase the likelihood of sustaining a distal humeral fracture include.
Elbow Problems
Make Your Appointment
- sports activities with increased risk of high-energy trauma
- risky driving style
- osteoporosis
Associations
- elbow dislocation
- floating elbow
- terrible triad injury
- neurovascular injury
Clinical presentation
Typical symptoms include pain and swelling of the elbow, instability and functional disability. Decreased or abnormal pulses might indicate a concomitant vascular injury. Weakness or paresthesias of the wrist might indicate nerve injury .
Complications
Trauma-related complications include the following :
- neurovascular injury
- forearm compartment syndrome
- Volkmann contracture
- osteoarthritis
Pathology
Distal humeral fractures can involve the epicondyles, the trochlea, the capitellum and the metaphysis of the distal humerus or all of those osseous structures.
Mechanism
Most distal humeral fractures are a result of a high energy trauma or a fall. Typical mechanisms include the following :
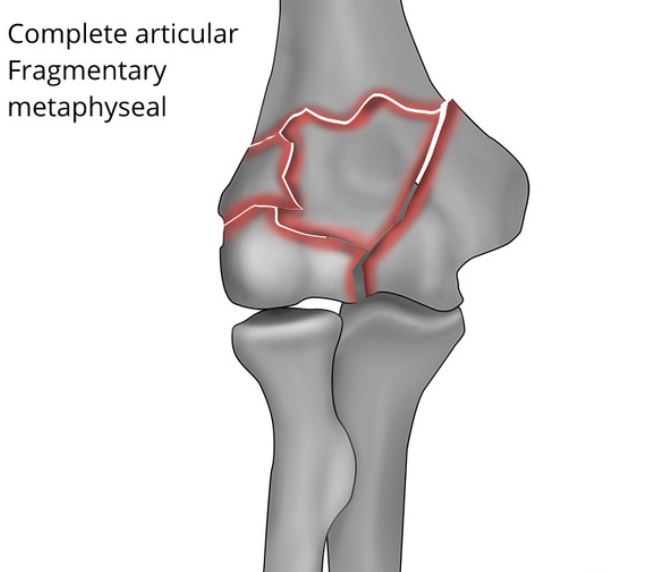
- direct impaction of the proximal ulna onto the trochlea or the capitellum, with the elbow in a flexed or extended position – this usually results in a complete articular fracture.
- indirect valgus or varus trauma in elbow extension – this usually results in a complete articular fracture.
- direct compression of the capitellar articular surface by the radial head either in extension or full flexion – results in an isolated capitellar fracture.
Radiographic Features
Fractures will usually show a radiolucency or cortical breach. Depending on how they are displaced there may be features of overlay and/or impaction.
Plain radiographs are the mainstay of diagnosis of distal humeral fractures. CT can be a helpful adjunct for the characterization of intra-articular fractures and surgical planning.
MRI is rarely needed in the acute setting can be helpful in concomitant ligamentous injuries.
Radiology Report
- fracture lines and plane
- location to the joint
- extra-articular, partial or complete articular
- involvement of the trochlea, the capitellum or both
- simple, fragmentary, multi-fragmentary
- signs of complications if evident (e.g. neurovascular injury)
Treatment and prognosis
Most distal humeral fractures are managed surgically since prolonged immobilization of one week or longer tends to lead to poor functional outcomes. The risk of prolonged fracture healing or fracture non-union is up to six times higher with conservative treatment than with surgery. Conversely, a good or excellent outcome has been shown for surgical fixation in long term follow-ups.
Non-operative, conservative management can be considered in stable non-displaced partial articular fractures (Milch type 1) and predominantly in low-demand patients with a high perioperative risk profile.
The primary goal of surgical treatment is an anatomical reconstruction of the articular surface and to gain stability to allow for early functional treatment for maintaining range of motion within the elbow joint. Open reduction and internal fixation with pre-contoured locking plates and headless compression screws are usually performed to achieve this goal.
Open fractures and fractures with neurovascular complications or associated compartment syndromes require an emergency operation.
There are different approaches with regard to the fracture type:
Epicondylar fractures are usually treated with screw fixation, for better rotational stability two screws can be used.
Extra-articular metaphyseal fractures are usually treated with preshaped locking plates and cortical screw fixation.
Partial articular fractures are usually managed with pre-contoured locking plates of the affected side and additional screw fixation 1. Coronal shear fractures can be managed with headless compression screws possibly accompanied by a pre-contoured locking plate if they are posteriorly comminuted.
Complete articular fractures are treated with a double-plate construction supplemented by additional metaphyseal screw fixation.
Very comminuted, non-reconstructable fractures or patients with pre-existing osteoarthritis or poor boine quality e.g. due to osteoporosis might need and profit from hemiarthroplasty or total elbow arthroplasty.
