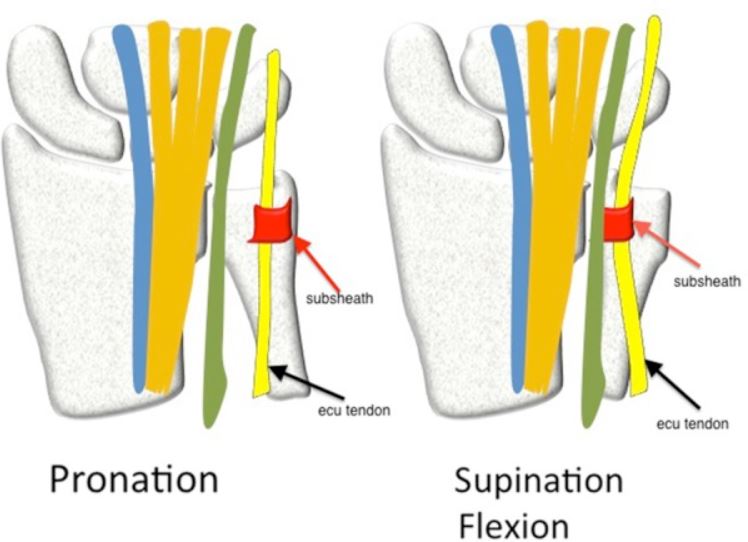
ECU subluxation / ECU Tenosynovitis
What is tenosynovitis?
Tenosynovitis (pronounced “ten-oh-sin-oh-vyt-us”) is inflammation of the thin layer of tissue (your synovial membrane) that surrounds your tendons. The condition can be painful and make it hard for you to move your joints like you usually can.
Your tendons are cords that connect your muscles to your bones. They let your bones move as you tighten and relax your muscles. Your synovial membrane is full of fluid. It protects your tendons and helps them move smoothly.
When something irritates, damages or infects your synovial membrane, inflammation can occur. In addition to symptoms from the tenosynovitis itself, this inflammation can lead to other serious issues if you don’t seek treatment. You’ll usually need to rest your affected tendon while it heals.
Types of tenosynovitis
Healthcare providers classify tenosynovitis in a few ways:
- Stenosing tenosynovitis. This type happens when inflammation around a tendon narrows the space in the tendon sheath, making it difficult for the tendon to move smoothly (stenosis). Examples include trigger finger and de Quervain’s tenosynovitis.
- Infectious tenosynovitis. A virus or bacterium that causes an infection in your tendon sheath can lead to this kind of tenosynovitis.
- Noninfectious inflammatory tenosynovitis. Overuse and autoimmune diseases like gout and rheumatoid arthritis can cause this type of tenosynovitis.
Symptoms and Causes
What are the symptoms of tenosynovitis?
The most common tenosynovitis symptoms include:
- Pain along the course of your tendon
- Swelling around your tendon
- Difficulty moving a part of your body like you usually can
- Pain when moving a part of your body
- Discoloration in a straight line along a tendon
WRIST PROBLEMS
- Distal Radius Fracture
- Distal Ulna Fracture
- Scaphoid Fracture, Nonunion
- Other Carpal Bone Fractures
- Dequervains Tenosynovitis
- Carpal Tunnel Syndrome
- Intersection Syndrome
- Swellings of Wrist Joint
- Ganglion Cyst
- Extensor Tenosynovitis
- Giant Cell Tumor of Distal Radius and Ulna
- Avascular Necrosis of Scaphoid
- Avascular Necrosis of Lunate (Keinbocks Disease)
- Distal RadioUlnar Joint & TFCC Injuries
- TFCC Tears (Acute & Chronic)
- DRUJ Instabilities & Dislocations
- Ulnocarpal Impaction Syndrome
- ECU Subluxation / ECU Tenosynovitis
- DISI (Dorsal Intercalated Carpal Instability)
- VISI (Volar Intercalated carpal Instability)
- SNAC Wrist (Scaphoid Nonunion Advanced Collapse)
- SLAC Wrist (Scapholunate Advanced Collapse)
- Lunate & Perilunate Dislocations
- Midcarpal Instabilities
- Radiocarpal Arthritis
- Mid-Carpal Arthritis
- Distal Radioulnar Joint Arthritis
Make Your Appointment
What does tenosynovitis feel like?
Tenosynovitis is usually painful. It can affect tendons connected to any muscle that helps one of your limbs push, pull, bend or straighten (your flexor and extensor muscles). You might also have trouble moving the affected part of your body like you usually can. The most common places tenosynovitis affects include your:
- Fingers
- Hands
- Wrists
- Feet
What causes tenosynovitis?
Tenosynovitis causes include:
- Autoimmune diseases. Any condition where your body’s defenses attack itself can cause damage to your synovial membrane.
- Overuse. Repeating one movement or motion constantly over a long period of time can lead to overuse syndrome. The damage from overuse syndrome often includes tenosynovitis.
- Infections. Many common infections can spread to your synovial membrane and lead to infectious tenosynovitis.
- Trauma. Any injury or accident that damages your tendons or the area around them can cause tenosynovitis.
Risk factors for tenosynovitis
Tenosynovitis can affect anyone. You’re more likely to develop tenosynovitis if you have:
- Rheumatoid arthritis
- Diabetes
- Hand infections
- Gout
- Thyroid disease
- Dupuytren’s disease
- Fibromyalgia
Complications of tenosynovitis
Tenosynovitis can be a serious condition because it can lead to complications, including:
- Joint stiffness
- Tendon rupture
- Necrosis (death) of the tendon tissue
- Adhesions (scar tissue)
- Need for amputation
Diagnosis and Tests
How is tenosynovitis diagnosed?
To diagnose tenosynovitis, your healthcare provider starts with a history and physical exam. They’ll check your symptoms and your range of motion (how far you can move a part of your body). They might also order blood tests or other labs to check for infections and inflammation.
What tests will be done to diagnose this condition?
After a physical exam, you might need at least one imaging test to confirm or show the extent of your disease. Imaging tests can also ensure there’s not another problem causing pain and stiffness, like a fracture or dislocation. These tests can include:
- X-rays. An X-ray can show any hardening (calcifications) of your synovial membrane and other signs of inflammation, like swelling.
- Magnetic resonance imaging (MRI) scan. Your provider might use an MRI to get a complete picture of your tendon and the area around it.
- Ultrasound. An ultrasound is like an X-ray for soft tissue. Your provider can use it to take pictures of the area around your tendon that will show any inflammation and areas of swelling.
- CT scan. A CT (computed tomography) scan will give your provider a more detailed picture of your tendon, bone and the surrounding soft tissue than an X-ray.
Management and Treatment
How is tenosynovitis treated?
How tenosynovitis is treated depends on what’s causing it. Tenosynovitis treatment can include:
- Rest and stopping the activity that caused the tenosynovitis
- Wearing a brace or splint to reduce stress on your tendon
- Applying heat or cold to the area to reduce pain or inflammation
- Oral steroids or steroid injections to calm down the inflammation
- Hand therapy to help decrease swelling and improve range of motion
- Surgery if an infection caused the tenosynovitis, or to open up areas of tightness that are restricting your tendons from moving normally
Your provider will tell you which specific treatments you’ll need based on how severe your symptoms are.
What medications are used to treat tenosynovitis?
Which medications you’ll need depends on the cause of the tenosynovitis. Some medications your provider might prescribe include:
- Antibiotics. If an infection caused the tenosynovitis, you’ll need antibiotics.
- NSAIDs. Over-the-counter NSAIDs like aspirin or ibuprofen can reduce pain and inflammation.
- Corticosteroids. Your provider might give you an injection or prescription of anti-inflammatory corticosteroids.
- Disease-modifying antirheumatic drugs (DMARDs). In people with inflammatory arthritis, these prescription medications can reduce pain and inflammation while protecting the joint from damage.
