Pediatric Steindler Flexuroplasty
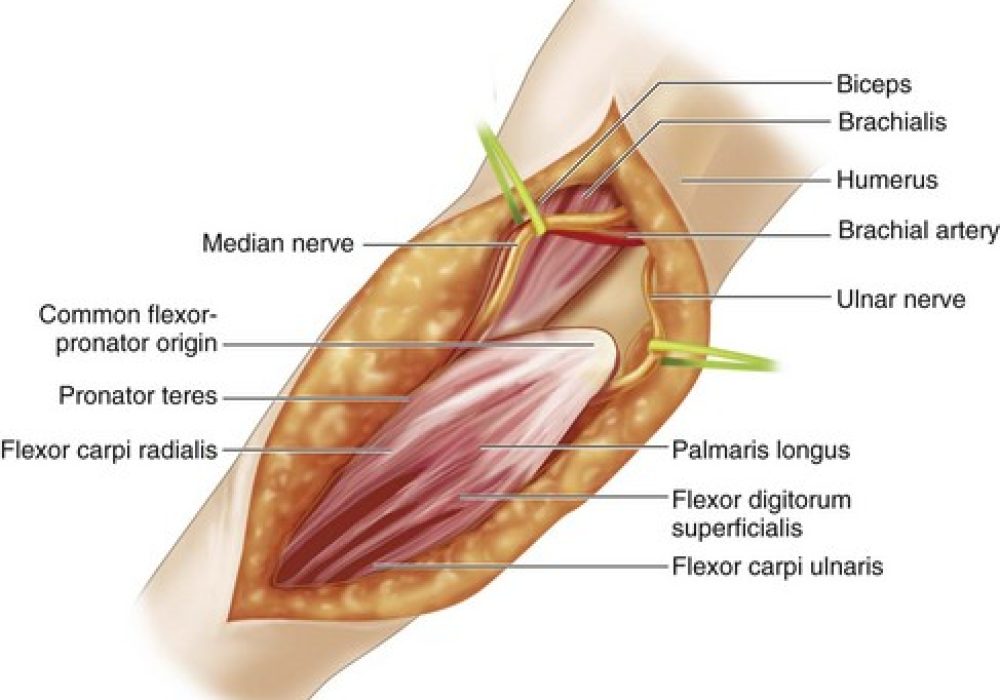
Pediatric Steindler Flexorplasty: Overview, Indications, Procedure, and Recovery
Steindler flexorplasty is a specialized surgical procedure used to restore elbow flexion in patients with paralysis or severe weakness of the biceps muscle. In pediatric patients, this technique is particularly valuable for children with brachial plexus injuries or other neuromuscular conditions that impair elbow flexion. By transferring the origin of the flexor-pronator muscle group proximally on the humerus, Steindler flexorplasty enhances the mechanical advantage of these muscles, allowing them to compensate for lost biceps function and restore active elbow flexion.
Brachial Plexus Surgery
- Nerve Grafting
- Distal Nerve Transfer – Oberlins Transfer, Somsacks Transfer, ICN to MCN Transfer, AIN to ECRB Transfer
- Tendon Transfers – LD to Biceps, Trapezius to Deltoid
- Free Functional Muscle transfer
- Pediatric Nerve Grafting
- Pediatric Distal nerve transfers
- Pediatric Distal nerve transfers
- Pediatric Contracture Release
- Pediatric Tendon Transfers
- Pediatric Steindler Flexuroplasty
Make Your Appointment
What Is Pediatric Steindler Flexorplasty?
Steindler flexorplasty is a tendon transfer procedure that involves repositioning the origin of the flexor-pronator muscle mass of the forearm from its normal location on the medial epicondyle of the humerus to a more proximal site on the humerus. This proximal transfer increases the lever arm and tension of these muscles, enabling them to flex the elbow more effectively. The procedure is typically reserved for children who have lost biceps function due to nerve injury or muscle paralysis but retain good wrist and hand function.
Indications for Pediatric Steindler Flexorplasty
Steindler flexorplasty is indicated in children with:
- Brachial plexus birth palsy: Resulting in biceps paralysis and loss of elbow flexion.
- Traumatic nerve injuries: Causing irreversible biceps muscle paralysis.
- Neuromuscular disorders: Leading to isolated elbow flexion weakness.
- Failed nerve repair or nerve transfer surgeries: Where biceps function has not been restored.
- Congenital muscle deficiencies: Affecting elbow flexion.
Advantages of Steindler Flexorplasty in Children
- Restores active elbow flexion without requiring nerve regeneration.
- Utilizes existing muscle groups with preserved function.
- Avoids the need for free muscle transfer in selected cases.
- Can be combined with other reconstructive procedures.
- Provides improved functional use of the upper limb.
Preoperative Evaluation
- Detailed clinical examination assessing elbow flexion strength, wrist and hand function.
- Electromyography (EMG) to evaluate muscle activity.
- Imaging studies such as X-rays to assess bone anatomy.
- Assessment of overall limb function and goals of surgery.
The Steindler Flexorplasty Procedure
Surgical Steps
- Anesthesia: General anesthesia is administered.
- Incision: A longitudinal incision is made over the medial aspect of the distal humerus and proximal forearm.
- Identification of Flexor-Pronator Mass: The flexor-pronator muscle group is carefully dissected from its origin at the medial epicondyle.
- Proximal Transfer: The origin of the flexor-pronator mass is detached and reattached more proximally on the humerus, typically 4 to 6 cm above the medial epicondyle.
- Fixation: The transferred muscle origin is secured to the humerus using sutures or bone anchors.
- Closure: The wound is closed in layers.
Duration
- The surgery typically lasts 2 to 3 hours.
Postoperative Care
Surgical Steps
- The arm is immobilized in a flexed position using a splint or cast for 4 to 6 weeks.
- Pain management and wound care are provided.
- Monitoring for complications such as infection or neurovascular injury.
Rehabilitation and Recovery
- After immobilization, physical therapy begins focusing on gradual range of motion exercises.
- Strengthening exercises for the transferred muscles are initiated.
- Functional training to improve elbow flexion during daily activities.
- Recovery of functional elbow flexion usually occurs within 3 to 6 months.
Risks and Complications
- Infection
- Neurovascular injury
- Failure of the transfer or loss of fixation
- Limited range of motion or stiffness
- Overcorrection or undercorrection of elbow flexion
- Donor site weakness or discomfort
Prognosis
- Pediatric patients generally have good outcomes due to their healing potential and adaptability.
- Most children achieve significant improvement in active elbow flexion.
- Early intervention and adherence to rehabilitation protocols enhance success.
When to See a Doctor
Parents should seek medical advice if their child has:
- Persistent inability to bend the elbow after nerve injury
- Weakness affecting daily activities
- Pain, swelling, or signs of infection after surgery
- Limited progress during rehabilitation
Conclusion
Pediatric Steindler flexorplasty is a valuable surgical option for restoring elbow flexion in children with biceps paralysis due to nerve injury or neuromuscular conditions. By repositioning the flexor-pronator muscle origin, this procedure enhances elbow flexion strength and improves upper limb function. Early evaluation by a pediatric orthopedic or nerve specialist and comprehensive rehabilitation are essential for optimal outcomes. If your child has difficulty bending the elbow due to muscle weakness or paralysis, consult a specialist to determine if Steindler flexorplasty is an appropriate treatment.
