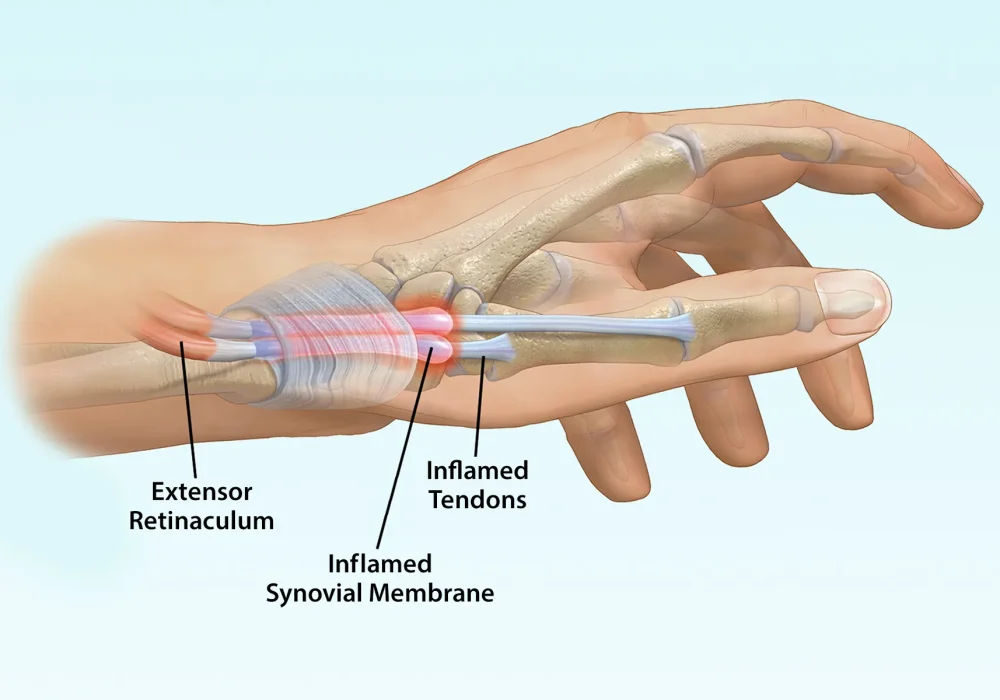
Joint & Tendon Synovitis
Rheumatoid Arthritis
Make Your Appointment
Joint and tendon synovitis is a medical condition characterized by inflammation of the synovial membrane, which lines the joints and tendon sheaths. This inflammation can cause pain, swelling, stiffness, and reduced mobility, significantly impacting a person’s quality of life. Understanding the causes, symptoms, diagnosis, and treatment options for synovitis is essential for effective management and recovery.
What is Synovitis?
Synovitis refers to the inflammation of the synovium, the thin layer of connective tissue that lines the inner surface of capsules of synovial joints and tendon sheaths. The synovium produces synovial fluid, which lubricates joints and tendons, facilitating smooth movement. When the synovium becomes inflamed, it thickens and produces excess fluid, leading to swelling and pain.
Synovitis can affect any synovial joint or tendon sheath but is most commonly seen in the knees, wrists, fingers, ankles, and shoulders. When it involves tendons, it is often referred to as tenosynovitis.
Causes of Joint & Tendon Synovitis
Several factors can trigger synovitis, including:
1. Injury or Trauma
Acute injuries such as sprains, strains, or fractures can cause synovial inflammation. Repetitive microtrauma from overuse, especially in athletes or manual laborers, can also lead to synovitis.
2. Infections
Bacterial, viral, or fungal infections can infect the synovial membrane, causing infectious synovitis. This condition requires prompt medical attention to prevent joint damage.
3. Autoimmune Diseases
Autoimmune disorders like rheumatoid arthritis, lupus, and psoriatic arthritis cause the immune system to attack the synovium, leading to chronic synovitis. This is often associated with joint destruction if untreated.
4. Crystal-Induced Arthritis
Conditions such as gout and pseudogout involve the deposition of crystals (uric acid or calcium pyrophosphate) in the joint, triggering synovial inflammation.
5. Other Causes
Other causes include metabolic disorders, allergic reactions, and idiopathic origins where no clear cause is identified.
Symptoms of Synovitis
The hallmark symptoms of joint and tendon synovitis include:
- Pain: Usually localized to the affected joint or tendon sheath, worsened by movement.
- Swelling: Due to excess synovial fluid and thickening of the synovium.
- Stiffness: Particularly after periods of rest or in the morning.
- Warmth and Redness: The inflamed area may feel warm and appear red.
- Reduced Range of Motion: Difficulty moving the joint or tendon fully.
- Tenderness: The affected area is often tender to touch.
In infectious synovitis, systemic symptoms such as fever and malaise may also be present.
Diagnosis
Diagnosing synovitis involves a combination of clinical evaluation, imaging, and laboratory tests.
Clinical Examination
A healthcare provider will assess the affected joint or tendon for swelling, tenderness, warmth, and range of motion. A detailed history including onset, duration, and associated symptoms is crucial.
Imaging Studies
- X-rays: Useful to rule out fractures or joint space narrowing.
- Ultrasound: Can detect synovial thickening and fluid accumulation.
- Magnetic Resonance Imaging (MRI): Provides detailed images of soft tissues, including synovium, tendons, and cartilage.
- Joint Aspiration: Fluid may be aspirated from the joint for analysis to detect infection, crystals, or inflammatory cells
Laboratory Tests
Blood tests may include markers of inflammation such as erythrocyte sedimentation rate (ESR) and C-reactive protein (CRP), rheumatoid factor (RF), anti-CCP antibodies, and tests for infections.
Treatment of Joint & Tendon Synovitis
Treatment depends on the underlying cause, severity, and duration of synovitis.
Conservative Management
- Rest: Avoiding activities that exacerbate symptoms.
- Ice and Compression: To reduce swelling and pain.
- Nonsteroidal Anti-Inflammatory Drugs (NSAIDs): Medications like ibuprofen reduce inflammation and pain.
- Physical Therapy: Gentle exercises to maintain joint mobility and strengthen surrounding muscles.
Medical Treatment
- Corticosteroid Injections: Direct injection into the joint or tendon sheath can rapidly reduce inflammation.
- Disease-Modifying Antirheumatic Drugs (DMARDs): Used in autoimmune synovitis to control the immune response.
- Antibiotics: Required for infectious synovitis.
Surgical Intervention
In cases where conservative and medical treatments fail, or if there is significant joint damage, surgical options may be considered:
- Synovectomy: Removal of inflamed synovial tissue.
- Arthroscopy: Minimally invasive procedure to clean the joint.
- Tendon Repair: If tendons are damaged.
Conclusion
Joint and tendon synovitis is a common yet potentially debilitating condition caused by inflammation of the synovial membrane. Understanding its causes, recognizing symptoms early, and seeking appropriate treatment can help manage the condition effectively. Advances in medical and surgical treatments have improved outcomes, allowing many individuals to maintain joint function and quality of life. If you experience symptoms suggestive of synovitis, consult a healthcare professional for a thorough evaluation and personalized care plan.
