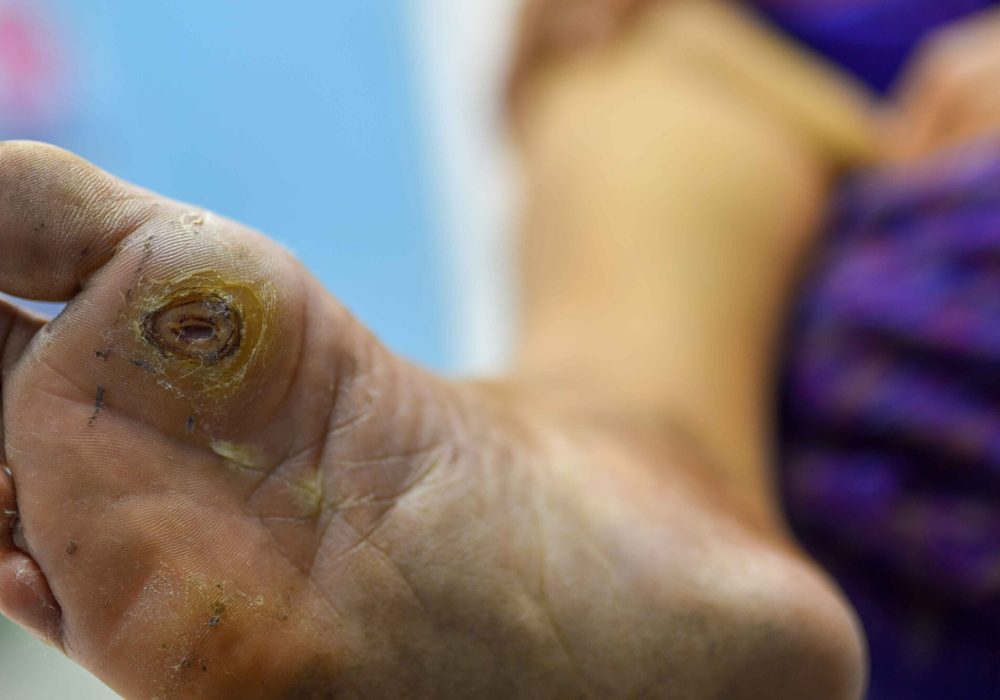
Diabetic Foot: Causes, Symptoms, Prevention, and Treatment
Diabetic foot is a serious complication of diabetes mellitus that affects millions of people worldwide. It encompasses a range of foot problems, including infections, ulcers, neuropathy, and poor circulation, which can lead to severe consequences such as amputation if not properly managed. Understanding the causes, symptoms, prevention strategies, and treatment options for diabetic foot is essential for patients and healthcare providers to reduce morbidity and improve quality of life.
Foot & Ankle Surgery
Make Your Appointment
What Is Diabetic Foot?
The term “diabetic foot” refers to any pathology of the foot directly related to diabetes. It primarily results from two major diabetes-related complications:
- Peripheral Neuropathy: Nerve damage causing loss of sensation, muscle weakness, and deformities.
- Peripheral Arterial Disease (PAD): Poor blood circulation leading to delayed wound healing and increased risk of infection.
These factors, combined with minor trauma or pressure, can cause foot ulcers and infections that may progress rapidly.
Causes of Diabetic Foot Problems
1. Peripheral Neuropathy
High blood sugar levels damage nerves over time, leading to:
- Loss of protective sensation (patients may not feel pain or injury)
- Motor neuropathy causing muscle weakness and foot deformities
- Autonomic neuropathy reducing sweat and oil production, leading to dry, cracked skin
2. Peripheral Arterial Disease (PAD)
Diabetes accelerates atherosclerosis, narrowing blood vessels and reducing blood flow to the feet. This impairs wound healing and increases the risk of infection.
3. Foot Deformities
Muscle imbalances from neuropathy can cause deformities such as claw toes or Charcot foot, increasing pressure points and risk of ulcers.
4. Trauma and Pressure
Minor injuries, ill-fitting shoes, or repetitive pressure can cause skin breakdown in insensitive feet.
5. Infection
Ulcers can become infected, leading to cellulitis, abscesses, osteomyelitis (bone infection), and gangrene.
Symptoms of Diabetic Foot Problems
- Numbness, tingling, or burning sensations in the feet
- Foot pain or weakness
- Changes in skin color or temperature
- Dry, cracked, or peeling skin
- Calluses or corns
- Open sores or ulcers, often painless
- Swelling or redness around wounds
- Foul odor or discharge from ulcers
- Fever or malaise in case of systemic infection
Diagnosis
1. Medical History and Physical Examination
Assessment includes checking for neuropathy, vascular status, foot deformities, skin integrity, and presence of ulcers or infections.
2. Neurological Tests
- Monofilament testing to assess protective sensation
- Vibration perception using tuning forks
- Pinprick and temperature sensation tests
3. Vascular Assessment
- Palpation of foot pulses
- Ankle-brachial index (ABI) to evaluate blood flow
- Doppler ultrasound or angiography for detailed vascular imaging
4. Laboratory and Imaging Studies
- Wound cultures to identify infections
- X-rays or MRI to detect bone involvement in osteomyelitis
Prevention of Diabetic Foot Complications
Prevention is key to reducing diabetic foot problems and includes:
1. Blood Sugar Control
Maintaining optimal glycemic levels slows nerve and vascular damage.
2. Regular Foot Care
- Daily inspection of feet for cuts, blisters, or abnormalities
- Keeping feet clean and moisturized (avoiding cracks)
- Proper nail trimming and callus management
- Avoiding walking barefoot
3. Appropriate Footwear
Wearing well-fitting shoes with adequate support and cushioning to prevent pressure points and injuries.
4. Routine Medical Checkups
Regular foot examinations by healthcare professionals to detect early signs of problems.
5. Smoking Cessation
Smoking worsens circulation and delays healing.
Treatment of Diabetic Foot Problems
Treatment depends on the severity and type of foot problem:
1. Neuropathy Management
- Optimizing blood sugar control
- Medications for neuropathic pain (e.g., gabapentin, duloxetine)
- Physical therapy to improve strength and balance
2. Wound Care
- Cleaning and debridement of ulcers to remove dead tissue
- Use of dressings that promote moist wound healing
- Offloading pressure using special footwear, casts, or braces
- Antibiotic therapy for infected wounds
3. Vascular Interventions
- Medications to improve blood flow
- Angioplasty or bypass surgery in cases of severe PAD
4. Surgical Treatment
- Correction of foot deformities to reduce pressure points
- Drainage of abscesses or removal of infected tissue
- Amputation in severe, non-healing infections or gangrene
5. Multidisciplinary Approach
Management often involves endocrinologists, podiatrists, vascular surgeons, infectious disease specialists, and wound care nurses.
Complications
If untreated, diabetic foot problems can lead to:
- Chronic non-healing ulcers
- Severe infections and sepsis
- Osteomyelitis
- Gangrene
- Lower limb amputation
- Reduced mobility and quality of life
Living with Diabetic Foot
Patients with diabetic foot problems should:
- Adhere strictly to treatment and preventive measures
- Monitor feet daily and report any changes promptly
- Maintain a healthy lifestyle with balanced diet and exercise
- Seek support from healthcare providers and support groups
When to See a Doctor
Immediate medical attention is necessary if you notice:
- New or worsening foot ulcers
- Signs of infection such as redness, swelling, warmth, or pus
- Persistent foot pain or numbness
- Changes in skin color or temperature
- Fever or systemic symptoms
Conclusion
Diabetic foot is a complex condition that requires vigilant prevention, early detection, and comprehensive management to avoid serious complications. With proper care, education, and multidisciplinary support, many patients can maintain foot health and prevent disability. Awareness and proactive measures are vital in reducing the burden of diabetic foot worldwide.
