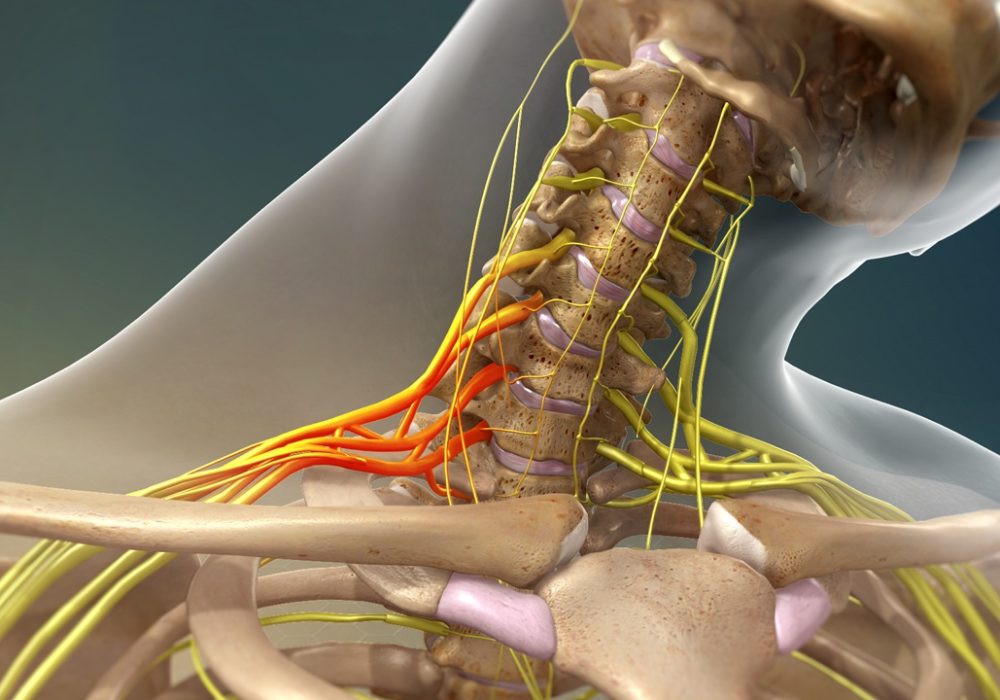
Adult and Pediatric Brachial Plexus Injuries
Brachial plexus injuries (BPIs) are complex nerve injuries that affect the network of nerves responsible for motor and sensory function of the shoulder, arm, and hand. These injuries can occur in both adults and children, but the causes, presentation, and treatment approaches often differ between these groups. Understanding the anatomy, mechanisms of injury, clinical features, and management options is crucial for optimizing outcomes in patients with brachial plexus injuries.
Anatomy of the Brachial Plexus
The brachial plexus is a network of nerves formed by the anterior rami of the spinal nerves C5 through T1. It is divided into roots, trunks, divisions, cords, and terminal branches. This intricate structure innervates the muscles and skin of the shoulder, arm, forearm, and hand. Damage to any part of this network can result in varying degrees of motor weakness, sensory loss, and functional impairment.
Brachial Plexus & Nerve Problems
- Adult & Pediatric Brachial Plexus Injuries
- Wrist & Finger Drop
- Claw Hand
- Foot Drop
- Nerve Compression
- Carpal Tunnel Syndrome
- Cubital Tunnel Syndrome
- Guyon’s canal Syndrome
- Pronator Syndrome
- Radial Tunnel Syndrome
- Wartenburg Syndrome
- Peroneal Nerve Compression
- Traumatic Brain Injury & Spastic Upperlimb
- Paralysis of Upper limb in Tetraplegic’s
- Thoracic Outlet Syndrome
Make Your Appointment
Causes of Brachial Plexus Injuries
Adult Brachial Plexus Injuries
In adults, brachial plexus injuries most commonly result from trauma. The typical causes include:
- Motor vehicle accidents: High-energy collisions can cause traction or avulsion injuries to the brachial plexus.
- Sports injuries: Contact sports or activities involving falls can lead to nerve stretch or compression.
- Penetrating trauma: Gunshot or stab wounds may directly damage the nerve structures.
- Iatrogenic injuries: Surgical procedures in the neck, shoulder, or chest can inadvertently injure the brachial plexus.
- Tumors or radiation: Neoplastic invasion or radiation fibrosis can cause compressive neuropathies.
Pediatric Brachial Plexus Injuries
In children, brachial plexus injuries are most often related to birth trauma, known as obstetric brachial plexus palsy (OBPP). This occurs during difficult deliveries, especially with:
- Shoulder dystocia: When the infant’s shoulder gets stuck behind the mother’s pelvic bone.
- Forceps or vacuum-assisted delivery: These instruments can exert traction on the infant’s neck and shoulder.
- Large birth weight: Macrosomia increases the risk of nerve stretch injuries.
Types of Brachial Plexus Injuries
Brachial plexus injuries are classified based on the severity and location of nerve damage:
- Neuropraxia: Mild injury with temporary conduction block; full recovery expected.
- Axonotmesis: Axonal damage with intact nerve sheath; recovery possible but slower.
- Neurotmesis: Complete nerve transection; requires surgical repair.
In addition, injuries can be:
- Pre-ganglionic (root avulsion): Nerve roots are torn from the spinal cord; often irreversible.
- Post-ganglionic: Injury distal to the dorsal root ganglion; better prognosis with repair.
Clinical Presentation
Adults
Symptoms depend on the level and extent of injury:
- Weakness or paralysis: In shoulder abduction, elbow flexion, wrist extension, or hand movements.
- Sensory loss: Numbness or tingling in the arm or hand.
- Pain: Neuropathic pain is common, often severe and difficult to manage.
- Muscle atrophy: In chronic cases due to denervation.
Pediatrics
In newborns, signs include:
- Flaccid arm: The affected limb may lie limp and motionless.
- Absent Moro reflex: The infant does not move the arm in response to startle.
- Asymmetric movement: One arm moves less or not at all compared to the other.
- Claw hand or wrist drop: Depending on the nerves involved.
Diagnosis
Diagnosis involves a combination of clinical examination and imaging studies:
- Physical examination: Assess motor function, sensory deficits, and reflexes.
- Electrodiagnostic studies: Nerve conduction studies and electromyography (EMG) help localize injury and assess severity.
- Imaging: MRI and CT myelography can visualize nerve root avulsions and soft tissue damage.
Treatment
Non-Surgical Management
- Physical therapy: To maintain joint mobility, prevent contractures, and strengthen muscles.
- Pain management: Medications including NSAIDs, neuropathic agents (gabapentin, pregabalin), and sometimes opioids.
- Occupational therapy: To improve functional use of the limb and adapt activities of daily living.
Surgical Management
Surgery is considered when there is no improvement after a period of observation (usually 3-6 months in children, earlier in adults) or in cases of severe injury:
- Nerve repair: Direct suturing of nerve ends if cleanly transected.
- Nerve grafting: Using autologous nerve segments to bridge gaps.
- Nerve transfers: Redirecting less important nerves to restore function to critical muscles.
- Muscle or tendon transfers: To restore movement when nerve repair is not possible.
- Free functional muscle transfer: Transplanting muscle with its nerve and blood supply.
Prognosis
The prognosis depends on the type, location, and severity of injury, as well as the timing and type of treatment:
- Adults: Recovery is often incomplete, especially in root avulsions. Early surgical intervention improves outcomes.
- Children: Many infants with OBPP recover spontaneously within the first few months. Those with persistent deficits benefit from early surgical evaluation.
Challenges and Advances
Brachial plexus injuries pose significant challenges due to the complexity of the nerve network and the critical functions involved. Recent advances include:
- Microsurgical techniques: Improved precision in nerve repair and grafting.
- Neurotrophic factors and nerve regeneration research: Enhancing nerve healing.
- 3D imaging and intraoperative nerve monitoring: Better surgical planning and outcomes.
- Multidisciplinary care: Combining neurology, orthopedics, physical therapy, and pain management.
Conclusion
Brachial plexus injuries in adults and children require timely diagnosis and a tailored treatment approach to maximize functional recovery. Awareness of the differences in etiology and presentation between these populations is essential for clinicians. With advances in surgical techniques and rehabilitation, many patients can regain significant function and improve their quality of life.
